The clients who come to this clinic with mould-related illness have usually done a great deal of the work already. They've identified the source — a roof leak, a flooded basement, a damp rental, a building that turned out to be sicker than it looked. They've remediated, or moved out, or both. They've worked with practitioners who actually understand the picture. They've taken binders. They've supported their methylation. They've cleared what could be cleared.
And in some cases, the recovery is slower than expected. Symptoms drop a level, then plateau. New flares appear without obvious triggers. Mornings feel worse than nights. The body keeps responding as if it is still encountering the thing it is supposedly clear of.
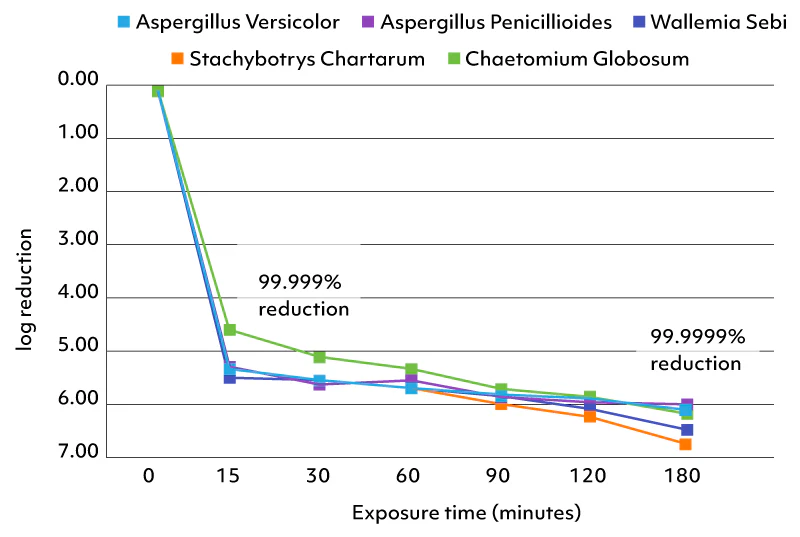
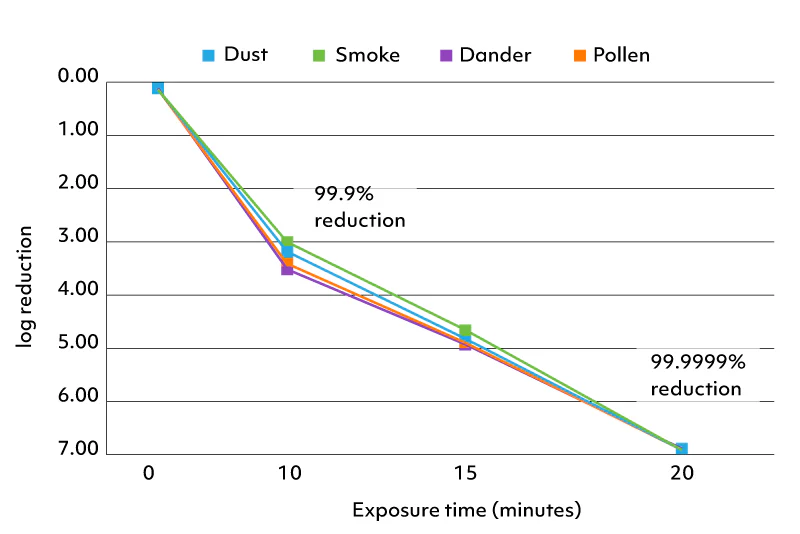
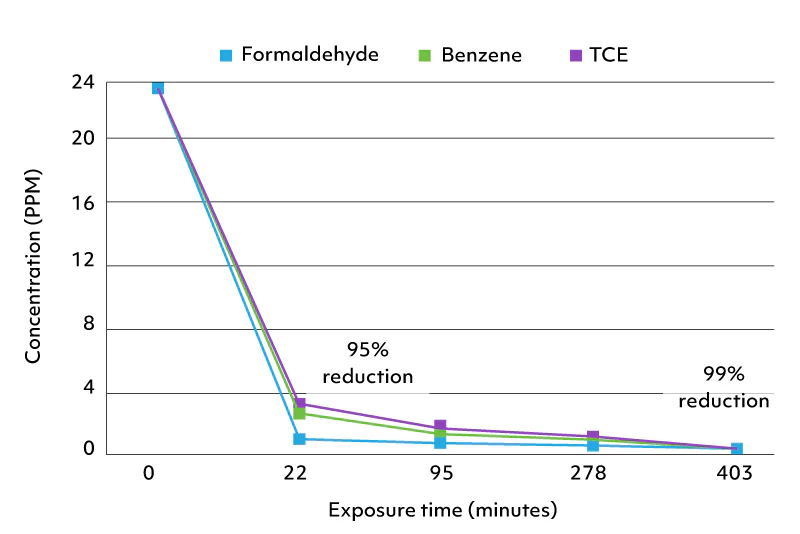
One of the most common explanations for this pattern is the air. Not the air in the building that caused the original injury — the air in the new, supposedly clean environment. Spores travel on shoes, on clothes, in HVAC ducts, on furniture. Mycotoxin-bound dust can persist in soft furnishings long after a building has been declared remediated. And in shared housing, in flats with neighbours, in older buildings of any kind in the UK and Ireland, the indoor air contains a baseline level of biological exposure that a sensitised person continues to react to.
The clients who plateau in their recovery are often the ones whose sleeping environment has not been addressed. The body cannot regulate inflammation while it is being re-challenged eight hours a night, every night, by the air it is breathing.